Keep Your Kidneys Healthy
Catch Kidney Disease Early
Your kidneys aren’t very big—each is about the size of your fist—but they do important work. They keep you healthy by maintaining just the right balance of water and other substances inside your body.
Unfortunately, if your kidneys start to malfunction, you might not realize it for a long while. Kidney disease usually doesn’t make you feel sick until the problem becomes serious and irreversible. March is National Kidney Month, a perfect time to learn more about how to keep your kidneys healthy and how to catch problems early.
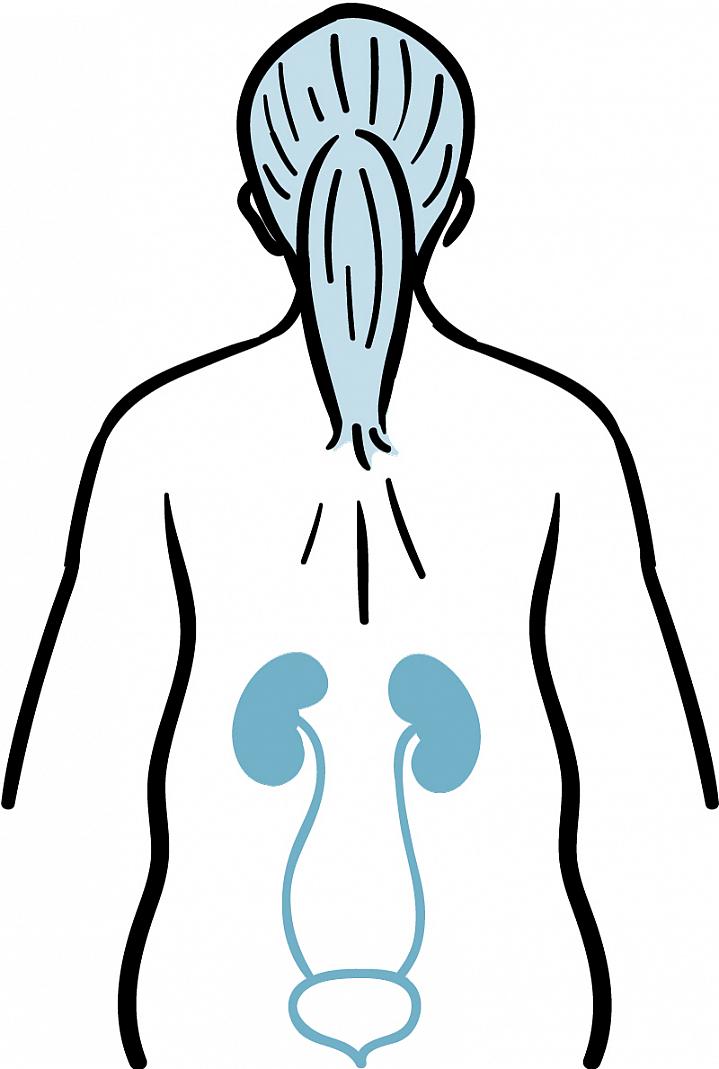
Your kidneys are 2 reddish, bean-shaped organs located on either side of your spine in the middle of your back. Their main job is to filter your blood. Each kidney contains about a million tiny filters that can process around 40 gallons of fluid every day—about enough to fill a house’s hot water heater. When blood passes through the kidney, the filters sift and hold onto the substances your body might need, such as certain nutrients and much of the water. Harmful wastes and extra water and nutrients are routed to the nearby bladder and flushed away as urine.
Your kidneys also produce several hormonesMolecules sent through the bloodstream to signal another part of the body to grow or react a certain way.. These hormones help to control your blood pressure, make red blood cells and activate vitamin D, which keeps your bones strong.
We all lose a little of our kidney function as we get older. People can even survive with just one kidney if they donate the other to a friend or family member.
But when kidney function drops because of an underlying kidney disease, it’s something to be concerned about. Toxins and extra water can build up in your blood. Falling hormone production can cause other problems. About 1 in 10 adults nationwide, or about 20 million people, have at least some signs of kidney damage.
There are different types of kidney disease. Most strike both kidneys at the same time, harming the tiny filters—called nephrons—and reducing their filtering ability. When damage to nephrons happens quickly, often because of injury or poisoning, it’s known as acute kidney injury. It’s more common, though, for nephrons to worsen slowly and silently for years or even decades. This is known as chronic kidney disease.
“Most people have few or no symptoms until chronic kidney disease is very advanced,” says Dr. Andrew Narva, a kidney specialist at NIH. “You can lose up to three-fourths of your kidney function and essentially have no symptoms.”
Chronic kidney disease can strike people of any race, but African Americans are especially at risk. African Americans also tend to have high rates of diabetes and high blood pressure, the 2 leading causes of kidney disease. Other risk factors for kidney disease include heart disease and a family history of kidney failure—a severe form of kidney disease.
If you have these risk factors, it’s important to be screened for kidney disease,” says Narva. “That usually involves simple laboratory tests: a urine test to look for kidney damage, and a blood test to measure how well the kidneys are working.”
The urine test checks for a protein called albumin, which isn’t routinely detected when your kidneys are healthy. The blood test checks your GFR—glomerular filtration rate. GFR is an estimate of your kidney’s filtering ability. A GFR below 60 is a sign of chronic kidney disease. A GFR below 15 is described as kidney failure.
“I tell my patients they should know their numbers,” says NIH kidney expert Dr. Jeffrey B. Kopp. “We usually cannot cure chronic kidney disease, but if we catch it early, we can slow down its progression.”
Without treatment, kidney disease often gets worse. If your GFR drops below 15, you may feel tired and weak, with nausea, vomiting and itching. By that point, you may need a kidney transplant or dialysis. It’s a good idea to talk with your doctor about the possibility of these therapies long before they’re needed. It takes time to understand your options, and it’s easier to figure things out when you’re feeling healthy.
“In general, the preferred therapy for kidney failure is to have a kidney transplant, but not everyone can have a transplant,” says Kopp. Some obstacles include long waiting lists for healthy kidneys and finding a well-matched donor.
Dialysis is a treatment that filters wastes and water from the blood, allowing patients with kidney failure to feel better and continue with everyday activities. NIH kidney specialist Dr. Paul Kimmel leads an NIH program to improve the lives of patients on dialysis. “Although dialysis is a life-saving therapy, it can be challenging for patients and families,” Kimmel says. “We’re encouraging researchers to explore innovative ways to improve the quality of life and long-term outcome for these patients.”
You can take many steps to avoid or delay reaching the point of kidney failure. The best thing you can do is control your blood pressure. A healthy lifestyle, including physical activity and a heart-healthy diet, can help to normalize blood pressure and also slow kidney disease.
“Most Americans eat more sodium and protein than the body needs. It’s your kidneys’ job to filter and get rid of the leftovers 24 hours a day, 7 days a week,” says registered dietitian Theresa Kuracina, who advises NIH on kidney health and nutrition. Healthy kidneys can generally handle the workload. “But if you have kidney damage, too much sodium and protein can have a negative effect,” Kuracina says. “We generally recommend eating less sodium and more fruits, vegetables and whole grains. To reduce fats, choose lean meats and low-fat or fat-free dairy products.”
If you have kidney disease, your health care provider may recommend additional changes to your diet. And if lifestyle changes aren’t enough to slow down kidney damage, your doctor may prescribe medications to reduce blood pressure, control blood glucose and lower your cholesterol.
Don’t wait to take the first step to keep your kidneys healthy. Talk to your health care provider about your kidneys, and ask if you should be tested for kidney disease.
NIH Office of Communications and Public Liaison
Building 31, Room 5B52
Bethesda, MD 20892-2094
nihnewsinhealth@od.nih.gov
Tel: 301-451-8224
Editor: Harrison Wein, Ph.D.
Managing Editor: Tianna Hicklin, Ph.D.
Illustrator: Alan Defibaugh
Attention Editors: Reprint our articles and illustrations in your own publication. Our material is not copyrighted. Please acknowledge NIH News in Health as the source and send us a copy.
For more consumer health news and information, visit health.nih.gov.
For wellness toolkits, visit www.nih.gov/wellnesstoolkits.



